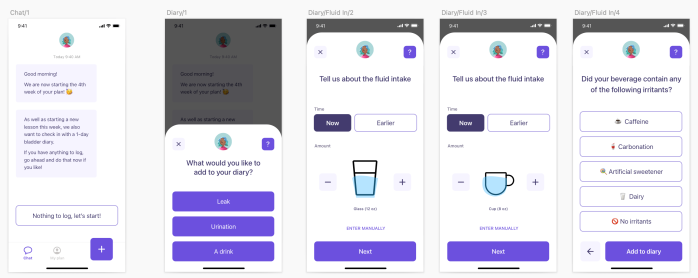
How regulators are making way for digital health
Rex’s panel also focused on policy and regulation in digital therapeutics. The panelists were excited about the ways regulation is catching up to the field’s rapid growth. One notable development is the FDA Modernization Act 2.0, which paves the way for computer-assisted and artificial intelligence data on new drugs to be accepted in place of data from animal testing.
This represents a regulatory paradigm shift, enabling more efficient and valid data generation for the safety and efficacy profiles of medical products and digital therapeutics.
It could also lead to more affordable drugs and therapeutics. Today, the average cost of developing a new drug is about $2.6 billion. Incorporating AI-driven data during regulatory processes could both reduce the cost and expedite approval, making life-saving treatments available sooner and to more people.
As digital therapeutics evolve, policymakers must balance the work of encouraging innovation and that of ensuring patient safety. Implementing robust data privacy laws and ethical guidelines is essential to protect patient data while leveraging the vast potential of digital health technologies.
Digital therapeutics today: already enhancing patient care
While the panelists spoke about the promise of digital therapeutics, they also discussed the real-world impact digital health products are already having.
Brian Feng, MD, Co-Founder and Chief Medical Officer of Evidence Care Doctor, provided a unique perspective as an emergency room physician. He stressed that digital therapeutics play a crucial role in empowering healthcare professionals with the latest evidence-based data to improve patient care. By integrating digital solutions into their workflows, he said, doctors and nurses can deliver better care, improving patient outcomes and financial results.
Indeed, a study published in the Journal of Medical Internet Research came to a similar conclusion: When digital therapeutics are used in chronic disease management…
In other words: digital health interventions led to better patient outcomes and significant cost savings for healthcare systems.
That digital therapeutics work so well for chronic illnesses in particular is especially encouraging, as chronic diseases account for about 75 percent of healthcare spending in the US.